Insulin Resistance: Causes, Symptoms, and How to Manage It
Insulin resistance is a common metabolic condition that often develops silently over time. Many people live with it for years without realizing it, even though it plays a major role in conditions such as type 2 diabetes, heart disease, and metabolic syndrome. Understanding insulin resistance is an important step toward protecting long-term health.
What Is Insulin Resistance?
Insulin is a hormone produced by the pancreas that helps move glucose (sugar) from the bloodstream into the body’s cells, where it is used for energy. Insulin resistance results from the body’s cells inability to respond properly to insulin.
When cells become resistant, the pancreas compensates by producing more insulin to keep blood sugar levels stable. Over time, this extra effort can strain the pancreas and lead to consistently high blood sugar levels. If insulin resistance continues unchecked, it can progress to prediabetes or type 2 diabetes.
Why Blood Sugar Can Look “Normal” At First
Early on, insulin resistance often hides behind “normal” fasting glucose or a normal A1C. High insulin levels can temporarily keep glucose controlled, even while the underlying problem grows.
That’s why you can feel off but still get lab results that don’t raise alarms. Early screening helps, especially if you have several risk factors, because you can make changes before blood sugar rises.
Insulin Resistance Vs. Diabetes, What’s The Difference?
Insulin resistance is the problem with how your body responds to insulin. Diabetes is the point where blood sugar stays high because insulin production can’t keep up, or insulin action is too weak.
Prediabetes sits in the middle. Blood sugar is higher than normal, but not high enough for a diabetes diagnosis. Insulin resistance is a major driver behind both prediabetes and type 2 diabetes, but it doesn’t guarantee you’ll develop either, especially if you act early.
What Causes Insulin Resistance, And Who Is Most at Risk?
Insulin resistance usually isn’t one thing. It’s a pile-up of factors; some you can change and some you can’t.
What Causes It
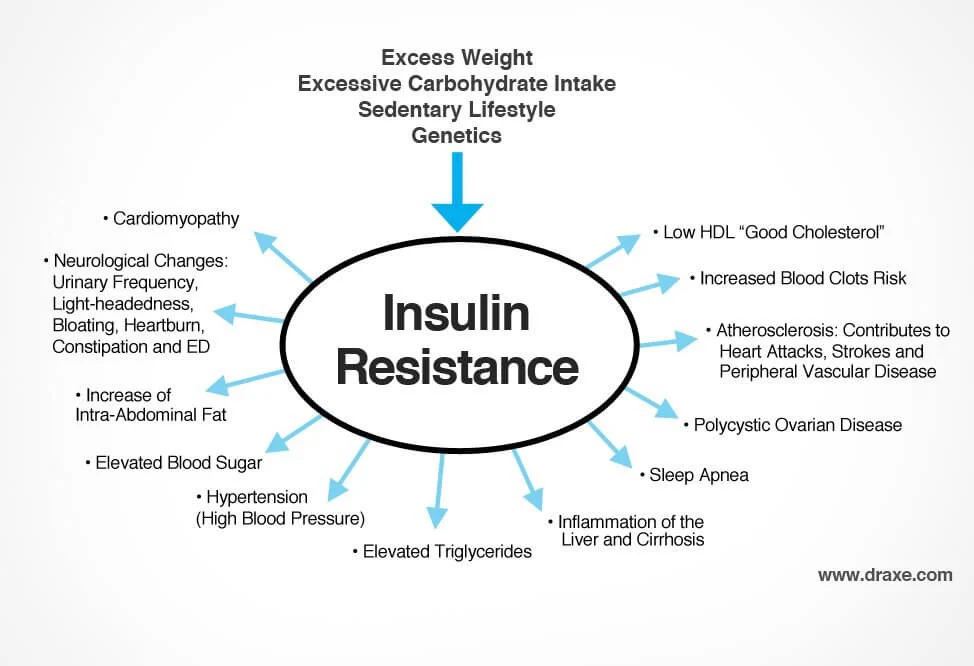
The most common drivers are excess body fat around the belly, low activity, and a long stretch of eating more calories than your body needs. Diet patterns high in added sugar and refined carbs can worsen the cycle, especially when fiber and protein are low.
Sleep and stress matter too. Lack of good sleep can make your body less receptive to insulin the next day. Long-term stress raises hormones that can push blood sugar higher and make cravings louder.
Genetics also plays a role, and risk is higher in some ethnic groups, including Black, Hispanic/Latino, Indigenous, and some Asian American populations.
Lifestyle Factors that Promote Insulin Resistance
Common lifestyle factors linked with insulin resistance include:
- Low movement (especially no strength training)
- High intake of sugary drinks and highly refined carbs
- Frequent overeating (even “healthy” foods can add up)
- Chronic short sleep
- High stress with little recovery time
- Smoking
- Heavy alcohol use
These factors can interfere with how insulin signals cells, making it harder for glucose to enter and be used effectively.
Health Conditions and Life Stages That Can Promote Insulin Resistance
Some health issues are associated with insulin resistance or make it more likely, such as fatty liver disease, blood pressure problems, and a cholesterol pattern of high triglycerides with low HDL.
Hormone-related conditions can also connect, including polycystic ovary syndrome (PCOS). Certain life stages like pregnancy (gestational diabetes risk) and menopause can shift metabolism and body fat distribution, which can affect insulin sensitivity.
If you suspect insulin resistance, it’s worth discussing your personal risk factors with a clinician, especially if you have a family history of type 2 diabetes.
Signs and symptoms
Many people have no obvious symptoms. When signs do show up, they often feel vague, like “something is off.” Pair that with normal-looking glucose early on, and it’s easy to miss.
The signs/symptoms
Some common symptoms include:
- Sleepiness or fatigue after meals, especially high-carb meals
- Cravings, especially for sweets or snack foods soon after eating
- Trouble losing weight, with more gain around the waist
- Darkened skin patches (often on the neck or armpits), sometimes linked with higher insulin levels
- Higher blood pressure
- Higher triglycerides
- Lower HDL
- A larger waist size
If you notice several of these, ask about screening. Depending on your situation, that might include fasting glucose, A1C, lipids, blood pressure, and waist measurement.
How to Minimize Insulin Resistance
You don’t need extreme rules. You need steady habits that make insulin’s job easier.
Start with these moves:
- Build meals around protein and fiber e.g. chicken, eggs, tofu, Greek yogurt, beans, lentils, veggies, and berries. Add healthy fats for staying power.
- Cut sugary drinks first such as soda, sweet coffee drinks, and juice. This one change can reduce big glucose spikes.
- Choose higher-fiber carbs, including oats, beans, whole grains, potatoes with skin, and keep refined carbs more occasional.
- Move after meals when you can, even 10 to 15 minutes of walking helps muscles use glucose.
- Do strength training 2 to 3 times per week, because more muscle often means better insulin sensitivity.
- Protect sleep with a consistent schedule. Aim for 7 to 9 hours.
- Lower stress in a realistic way, such as daily walks, breath work, therapy, or a no-phone wind-down.
Even modest weight loss, often 5 to 10 percent if you’re above your healthy range, especially from the belly area, can improve insulin sensitivity.
Treatment options for Insulin Resistance
Treatment depends on your tests, symptoms, and risk. For many people, it requires lifestyle, food quality, strength training, and weight loss if needed.
Your clinician may also discuss medication in certain cases, such as drugs that improve insulin resistance or help prevent progression to type 2 diabetes in higher-risk patients. Some newer weight-loss medications can improve insulin resistance by helping reduce excess body fat, but they’re not a DIY solution and aren’t right for everyone.
Monitoring matters. Ask what follow-up makes sense for you, which may include A1C, fasting glucose, lipids, and blood pressure.
Conclusion
Insulin resistance is common, often quiet, and it doesn’t have to be a one-way road. The biggest levers are simple and repeatable—move more, cut added sugar and ultra-processed foods, prioritize sleep, and aim for gradual waist fat reduction if needed.
Pick one change to start this week, like a 10-minute walk after dinner or swapping sugary drinks for water. If you have multiple risk factors or persistent symptoms, schedule a check-in with a clinician and ask about screening. Small steps, repeated, can shift the story.
Frequently Asked Questions
Who is at risk of developing insulin resistance?
People who are inactive, have excess abdominal fat, a family history of diabetes, or long-term stress are at higher risk.
Does insulin resistance cause weight gain?
Insulin resistance can make weight management more difficult because the body struggles to use glucose efficiently.
Can insulin resistance affect energy levels?
Yes, when cells do not absorb glucose properly, it can lead to fatigue and low energy throughout the day.
Are medications always needed for insulin resistance?
Not always. Many people can manage insulin resistance with lifestyle changes, though some may need medication based on medical advice.
How long does it take to improve insulin resistance?
Improvement varies by individual, but consistent healthy habits can lead to positive changes over time.








