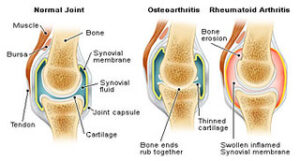
Rheumatoid arthritis (RA) is a chronic autoimmune disease that mainly affects the joints but can also impact many other body systems. Unlike osteoarthritis, which develops due to wear and tear, rheumatoid arthritis occurs when the immune system mistakenly attacks healthy tissues, leading to inflammation, pain, and progressive joint damage.
RA affects millions of people worldwide and is more common in women than men. It can occur at any age, but most often it begins between the ages of 30 and 60. Early diagnosis and proper treatment are essential to slowing disease progression, preserving joint function, and maintaining quality life.
What is Rheumatoid Arthritis?
Rheumatoid arthritis is a systematic inflammatory autoimmune condition. The condition occurs when the immune system fails to work properly and targets the synovium, which is the lining of the membranes that surround joints. This leads to swelling, warmth, pain, and stiffness. Over time, chronic inflammation can damage cartilage, bone, and connective tissues, leading to joint deformity and loss of function.
Because RA is systematic, it not only affects joints, but also organs such as the heart, eyes, lungs, skin, and blood vessels. This makes it a complex and potentially serious condition.
Common Symptoms of Rheumatoid Arthritis
Symptoms of rheumatoid arthritis can vary widely in severity and may come and go in periods known as flares and remissions. Early signs are often subtle, which can delay in diagnosis.
Symptoms may include:
• Morning stiffness lasting longer than 30-60 minutes
• Fatigue
• Weakness
• Reduced range of motion
• Pain, swelling, stiffness, and tenderness in multiple joints
• General feeling of illness (malaise)
• Loss of appetite
• Fatigue and low energy
RA most commonly affects the small joints of the hands, wrists, and feet, but larger joints such as the knees, shoulders, hips, and elbows may also be involved.
Causes and Risk Factors of RA
The exact cause of rheumatoid arthritis is unknown, but researchers believe that it results from a combination of genetic, environmental, and hormonal factors.
Genetics
Certain genes, particularly those related to the human leukocyte antigen (HLA) system, increase the risk of developing rheumatoid arthritis. Having a family member with rheumatoid arthritis also increase the likelihood of developing the condition.
Environmental Triggers
Factors such as smoking, exposure to air pollution, and certain infections may trigger immune responses.
Hormonal Factors
RA is more common is women, suggesting that hormones such as estrogen may play a role. It’s more likely for the symptoms to change during menopause and pregnancy.
Lifestyle Factors
Poor diet is one of the supposed causes of RA. If you consume a lot of red meat and have low intake of vitamin C then you are highly susceptible to developing this condition. Also, other lifestyle factors like obesity, lack of physical activity, and chronic stress can lead to RA.
How Rheumatoid Arthritis is Diagnosed
Diagnosing rheumatoid arthritis can be challenging, especially in the early stages. This is because there’s no single test that confirms it. therefore, doctors rely in a combination of clinical evaluation and diagnostic tests.
Medical History and Physical Exam
The healthcare provider assesses the symptoms such as stiffness, joint swelling, and functional limitations. They’ll also review family history and lifestyle factors.
Blood Tests
There a few blood tests that can show possible signs of rheumatoid arthritis:
Erythrocyte Sedimentation Rate (ESR)
The physician takes a sample of red blood cells and puts them in a test tube with a testing agent. A timer is set to see how long it takes for them to get to the bottom of the tube. If they sink faster than usual, there is likely some type of inflammation. And possibly rheumatoid arthritis may be one of the causes.
C-reactive Protein (CRP)
The tests show the presence of inflammation in the body by checking how much CRP there is in the blood. More CRP confirms inflammation.
Rheumatoid Factor and Anti-CCP Antibodies
When RA starts, most people have a rheumatoid factor in their blood. Also, people who test positive for anti-CCP are likely to get rheumatoid arthritis.
Imaging Tests
Doctors will conduct x-rays to assess joint damage, ultrasound to detect early inflammation, and MRI for detailed images of the soft tissues and joints. Early diagnosis is important, as starting treatment early can significantly slow disease progression.
Complications of Rheumatoid Arthritis
RA increases the risk of developing serious conditions like:
• Osteoporosis: RA itself, and some of the medication used for its treatment, can increase the risk of osteoporosis. This is a condition which weakens the bones and makes them more brittle.
• Rheumatoid nodules: These are firm bumps of tissue that mostly form around the pressure joints, such as the elbows. However, these nodules can form anywhere in the body, including the lungs and heart.
• Infections: RA and its medications can harm the immune system, which leads to more infections.
• Dry eyes and mouth: People with RA are more likely to develop conditions that lower the amount of moisture in their eyes and mouth. This is known as secondary Sjogren’s syndrome.
• Lung disease: Individuals with rheumatoid arthritis are at a higher risk of inflammation of lung tissues. This can result in scarring and lead to shortness of breath that gets worse over time.
• Carpal tunnel syndrome: If RA affects the wrists, the swelling can press on the nerve leading to the hand and fingers.
• Heart problems: It can increase the risk of hardened and blocked arteries and also inflammation of the sac around the heart.
• Lymphoma: Rheumatoid arthritis is likely to raise the risk of group cancers that happen in the lymph system or lymphoma. It can also lead to other types of cancer.
Regular monitoring and comprehensive care can reduce the risk of these complications.
Treatment Options
Although there is no cure for rheumatoid arthritis, many effective treatments are available to control symptoms, reduce inflammation, prevent joint damage, and improve quality of life.
- Disease-Modifying Antirheumatic Drugs (DMARDs): These slow the progression of the disease and prevent joint damage. Common examples include sulfasalazine, methotrexate, and leflunomide.
- Biologic DMARDs: Biologics target specific components of the immune system and are often used when conventional DMARDs are not effective. Examples include TNF inhibitors and interleukin inhibitors.
- Janus Kinase (JAK) Inhibitors: These are oral medications that block specific pathways involved in inflammation and are a good option for moderate to severe RA.
- Nonsteroidal Anti-inflammatory Drugs (NSAIDs): For relieving pain and reducing inflammation, they don’t slow disease progression.
- Corticosteroids: Steroids may be used as short-term relieve of severe inflammation and flares.
How to Manage the Symptoms
Lifestyle changes play a key role in managing rheumatoid arthritis. Some ways that you can manage the condition include:
Regular low-impact exercises to help maintain joint flexibility, muscle strength, and overall health. You can do simple exercises like swimming, walking, cycling, stretching, and yoga.
Including an anti-inflammatory diet in your meal plans. Ensure that your meal includes omega-3 fatty acids from flaxseed or fish, fruits and vegetables rich in antioxidants, and less processed foods and added sugars. It is also good to maintain a healthy weight.
Manage your stress levels as chronic stress can worsen RA symptoms. Techniques such as deep breathing, meditation, and mindfulness may help manage stress levels.
Conclusion
Rheumatoid arthritis is a complex autoimmune condition that affects both joints and overall health. Early diagnosis, appropriate medical treatment, and healthy lifestyle choices are key to managing the condition effectively. If you suspect symptoms of rheumatoid arthritis, seeking early medical advice can make a significant difference in long-term outcomes.
Frequently Asked Questions (FAQs)
Q1. What is the life expectancy of a person with rheumatoid arthritis?
Rheumatoid arthritis life expectancy is 26. Years after diagnosis. However, a lot depends on the type of treatment one gets after the diagnosis.
Q2. Does rheumatoid arthritis ever go away?
Unfortunately, there’s no cure for rheumatoid arthritis. However, early diagnosis and appropriate treatment enable many people with this condition to have periods of months or years between flares. This way, they can lead full lives and even continue with regular employment.
Q3. What worsens rheumatoid arthritis?
Not sticking to your RA treatment will worsen the condition. If you fail to fill prescriptions, take medications as directed, exercise, or skip appointments, then the risk of worsening symptoms increases.
Q4. What are the four stages of rheumatoid arthritis?
The four stages of RA are: Stage I- early synovitis, Stage II- moderate joint space narrowing and periarticular bone loss, Stage III- severe erosions and deformities, and Stage IV- end stage characterized by collapse with major loss of function.
Q5. What is the biggest indicator of rheumatoid arthritis?
The main symptoms of RA are swelling, stiffness, and joint pain. You may experience more general symptoms and inflammations in other body parts. Normally, the symptoms develop gradually over several weeks, but in some cases can progress quickly over a number of days.
Further Reading Resources
- National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS) - Rheumatoid Arthritis: Causes, Diagnosis, and Treatment (https://www.niams.nih.gov/health-topics/rheumatoid-arthritis)
- Mayo Clinic - Rheumatoid Arthritis – Symptoms and Causes (https://www.mayoclinic.org/diseases-conditions/rheumatoid-arthritis)
- Arthritis Foundation - Rheumatoid Arthritis Symptoms, Treatment, and Lifestyle Guidance (https://www.arthritis.org/diseases/rheumatoid-arthritis)